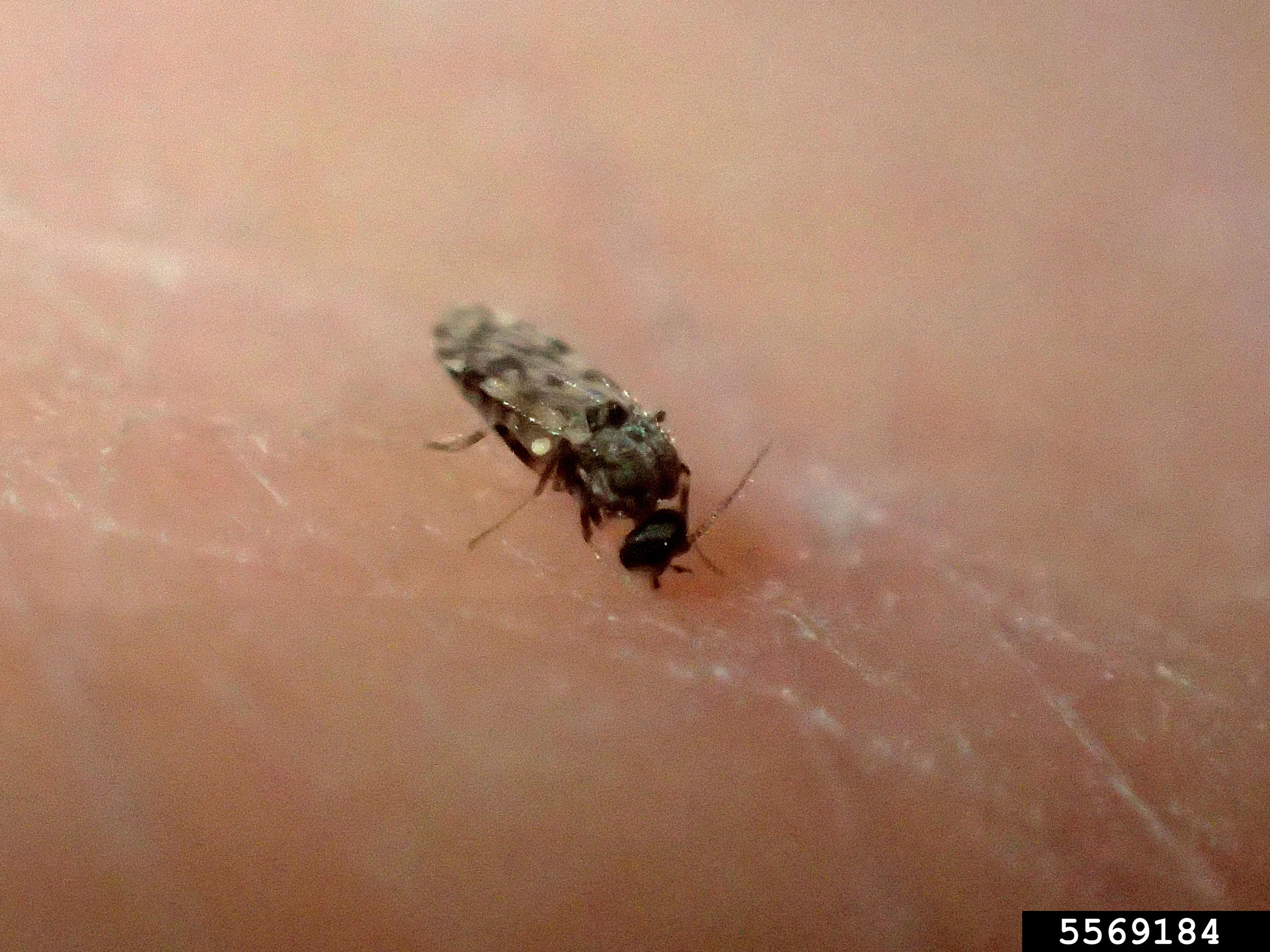
Equine insect bite hypersensitivity (IBH) goes by many names: Queensland Itch, sweet itch or summer eczema. Seasonal episodes of itching misery felt by affected horses cause them to scratch and traumatize their manes, tails and chests down to bleeding tissue. The Culicoides biting midges responsible for this allergic reaction inject salivary proteins as they feed that can elicit Type 1 and 4 allergic responses in predisposed horses.
Solutions to manage this skin condition rely on relocation to low-risk habitats with less exposure to the midges; stabling with protective screens during the dawn and dusk prime feeding hours of midges; and keeping horses in open, windy locations and away from wooded areas and standing water that is a breeding habitat. In addition, the use of custom-designed fly sheets and insect repellants help thwart the midges. Many of these are time-consuming strategies that require effort and compliance by the horse owner. Pharmaceutical control measures rely on systemic treatment with glucocorticoids and/or antihistamines, although antihistamines tend to have limited efficacy.
ASIT Therapy
Another possible therapeutic approach is the use of allergen-specific immunotherapy (ASIT) in a manner similar to treating humans to mitigate immune responses to seasonal allergens. ASIT works by producing IgG antibodies that block binding of allergen-specific IgE antibodies to the allergens in addition to decreasing production of specific cytokines that spark an immune reaction.
Three different studies have attempted ASIT for IBH by using whole body extract of Culicoides midges. In those trials, there was no significant improvement in clinical signs of horses treated with IBH ASIT compared to a placebo group, likely due to the inclusion of only a very small fraction of the salivary gland proteins that stimulate the allergic response [Jonsdottir, S.; Cvitas, I.; Svansson, V.; et al. New Strategies for Prevention and Treatment of Insect Bit Hypersensitivity in Horses. Current Dermatology Reports 2019, vol. 8, pp. 303-312; doi.org/10.1007/s13671-019-00279-w].
Research on Concentrated Allergens
Further attempts to isolate the causative allergens of IBH has led to more concentrated purification of the most relevant Culicoides allergens. For high-risk individuals—based on genetic predisposition and breed, such as Icelandic horses, Friesian horses, Shetland ponies, and Belgian Warmbloods—preventive immunotherapy might be useful prior to development of sensitization. This approach is still in developmental stages. A study on the use of this purified material as a prophylactic treatment via either intralymphatic or intradermal injection was performed on healthy Icelandic horses not previously exposed to the midges. The intralymphatic route of administration resulted in a stronger antibody response than intradermal injection.
SLIT Administration
Sublingual immunotherapy (SLIT) is another route of administration under investigation. A trial of this approach was used in four horses treated six times over 20 weeks by using a special bit to contact the oral mucosa. An initial weak IgG response was enhanced by a booster eight months later. This second IgG response had some blocking activity on allergen proteins, and these allergen-specific antibodies were detectable in saliva.
Role of Eosinophils
In addition, eosinophils are significant in IBH as they accumulate in IBH skin lesions and elevate in peripheral blood. There is ongoing research into “vaccines” that target interleukin-5 (IL-5) and IL-31.
Other Studies
Other studies are focusing on possible defects in the epithelial barrier in horses suffering from IBH. Researchers believe that within skin lesions of IBH horses, there is disruption in tight junctions, epidermal thickening, disruption of the epithelial barrier, and lipid metabolism impairment of the epithelium. These findings present an opportunity to explore new therapeutic targets to achieve more than palliative treatment [Cvitas, I.; Oberhansli, S.; Leeb, T.; et al. Investigating the epithelial barrier and immune signatures in the pathogenesis of equine insect bite hypersensitivity. PLoS ONE 2020, 15(4): e0232189; doi.org/10.1371/journal.pone.0232189].
The presence of allergic hypersensitivity might not be solely confined to the skin in horses with IBH. A Swiss study of 69 horses showed IBH-associated airway hyperreactivity even in the absence of inhaled allergens or overt clinical respiratory signs. This multi-allergic response is recognized in humans, cats and dogs where two-thirds of patients with atopic dermatitis later develop allergic rhinitis while half progress to asthma [Lanz, S.; Brunner, A.; Graubner, C.; et al. Journal of Veterinary Internal Medicine 2017, vol. 31, pp. 1877-1883; DOI: 10.1111/jvim.14817]. The study identifying multi-hypersensitivity responses summarized that “horses suffering from IBH have a higher risk for airway hyperreactivity and therefore may be predisposed to develop equine asthma in future.“








