This article originally appeared in the Winter 2025 issue of EquiManagement. Sign up here for a FREE subscription to EquiManagement’s quarterly digital or print magazine and any special issues.
Tucked away out of sight, postoperative incisional infections can become persistent problems that negatively affect a colic patient’s outcome more often than nonsurvival. This article highlights the prevalence of incisional infections, contributing factors, antimicrobial stewardship, and steps surgeons are taking to minimize them.
Prevalence Reports
Most studies on incisional infections cite a wide prevalence of 7-43%. This range is wide because different studies use different definitions of infection, says Theunis Griessel, BVSc, MSc, MRCVS, resident of equine surgery in the Department of Clinical Animal Studies at Onderstepoort Faculty of Veterinary Science, University of Pretoria, in South Africa. Some, for example, include any type of incisional drainage, whereas others only include purulent discharge or diagnosis based on culture results.
Dean Hendrickson, DVM, MS, DACVS, professor of surgery at Colorado State University’s College of Veterinary Medicine and Biomedical Sciences, believes incisional infections should be diagnosed based on culture. “It is a travesty that with all we know about antimicrobial stewardship that we just empirically start them on antibiotics,” he says.
In a 2024 study, Griessel et al. considered an incision infected if it had any purulent or serous discharge for more than 24 hours during hospitalization. Based on that definition, infection prevalence following colic surgery in 143 horses was 26.6%. This is similar to the 28.7% prevalence Isgren et al. reported in 2024 and 33% by Gandini et al. (2024) but much higher than the prevalence of 12.8% reported by Crabtree et al. (2025).
Sequelae of Incisional Infections
In Griessel’s study, incisional infections developed a mean of 9.5 days postoperatively, with a standard deviation of 7.1 days. Isgren et al.’s results were similar, with infections developing at a mean of 9.7 days, with a standard deviation of 4.6.
“This means that many incisional infections are diagnosed by the primary practitioner after the horse has been discharged from the hospital,” notes Hendrickson.
To evaluate incisional infections on the farm, he recommends first assessing the extent of the infection with ultrasound. “Then a culture should be taken and some of the skin sutures/staples removed to allow drainage,” he adds. “Cytology can be done to confirm bacterial presence and get an idea if they are Gram-positive or negative.”
Why Should Practitioners Be So Aggressive?
Incisional infections following colic surgery delay healing and might contribute to postoperative discomfort, increased treatment costs, and extended hospitalization (if diagnosed in the hospital or having to return for additional treatment).
“In our study, horses with incisional infections were hospitalized for 10 days longer than horses without infections,” says Griessel.
Incisional infections also increase the risk of abdominal herniation: Horses with incisional infections are four to nine times more likely to develop incisional hernias. Griessel et al. found a 7.17-fold increase in herniation in horses with incisional infections. Horses with herniation are seven to 14 times less likely to return to athletic function following surgery.
Factors Contributing to Incisional Infections
Veterinarians have proposed many factors that predispose horses to incision infections, but few have been substantiated through clinical trials. Potential contributors might include:
- Horse’s age.
- Concomitant disease.
- Increased body weight.
- Surgical preparation.
- Surgeon experience.
- Type and duration of surgery.
- Surgical environment.
- Duration of colic prior to surgery.
- Severity of colic.
- Preoperative packed cell volume > 48% or heart rate > 60 beats per minute.
- Pain at time of admission.
- Intraoperative hypothermia and hypoxia.
Some pertinent predisposing factors include suture pattern used for incisional closure/closure method, incision length more than 27 centimeters, and use and type of abdominal bandage (Griessel et al. 2024, Cerullo et al. 2025).
In Griessel’s surgical suite, the linea alba is closed with a simple continuous suture pattern. “There have been studies investigating the use of simple interrupted or vertical mattress suture techniques for closing of the linea alba rather than the standard simple continuous suture technique,” he says. “These studies found that using the simple interrupted or a combination of simple interrupted and vertical mattress suture patterns resulted in a lower rate of incisional infection. However, these are time-consuming to perform and not often used.”
How and When Do Incisions Become Contaminated?
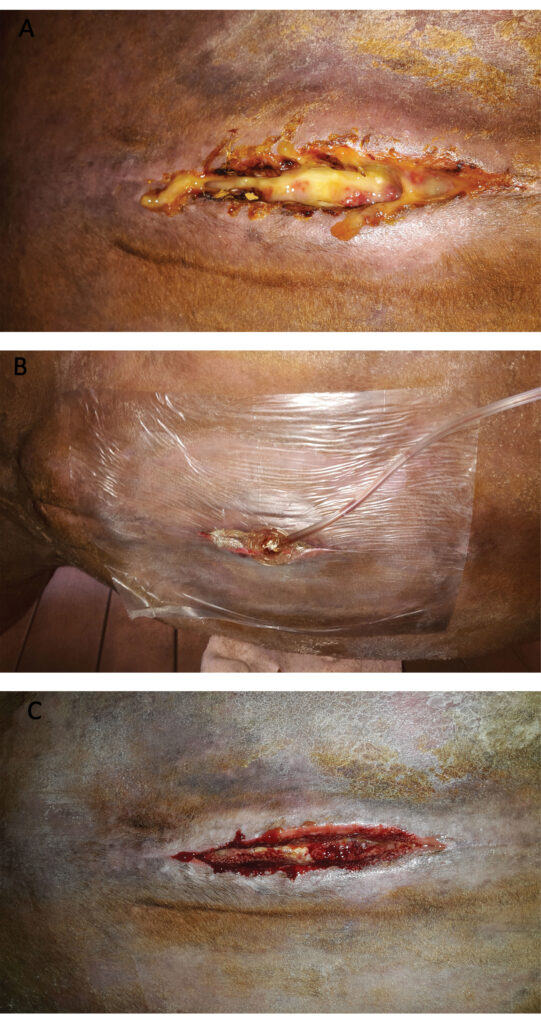
According to Isgren et al., surgical site infections can be reduced by “minimizing bacterial contamination of the incision intraoperatively and during the early postoperative period, particularly during anesthesia recovery.”
This makes sense since bacterial contamination of the surgery site is required for infection to occur. But simply having bacteria at the surgical site does not mean an infection will develop. For example, virulence of the invading pathogen and pathogen load, host characteristics (immune status, age), and tissue/wound characteristics all play roles in infection development (Cerullo et al. 2025).
Many routine colic surgeries are typically classified as clean (e.g., volvulus) or clean-contaminated (e.g., resection and anastomosis), and incisions are considered clean at the start of surgery. But according to Cerullo et al., wounds aren’t still clean at the end of surgery. In that study, 70 horses undergoing colic surgery had their surgery site swabbed preoperatively and were negative for bacterial growth. Following surgery, a bacterial swab, biopsy, or fine-needle aspiration of the wound edges was performed on each horse. Of the clean surgeries, 49.1% had bacterial contamination, which was higher than the 41.2% of incisions from clean-contaminated surgeries.
Alternatively, Salciccia et al. (2024) suggest that incisional infections occur during recovery, particularly if the recovery was poor (e.g., a sweaty horse on a dirty recovery stall floor).
In their study, Griessel et al. swabbed 24 of the 38 horses that developed incisional infections. The most common bacterial isolates were Escherichia coli, Staphylococcus spp., Enterococcus spp., Pseudomonas spp., Salmonella spp., and Enterobacter spp., which are predominantly considered commensals and environmental contaminants.
Interventions Aimed at Decreasing Incisional Infections
Antibiotics
Several recently published studies examined antibiotics’ effects on incisional infections. Guidelines in veterinary medicine support the concept that antibiotics should be administered for the shortest effective duration to minimize development of resistance to pathogens. In humans, antimicrobial use beyond 24 hours postoperatively did not reduce the risk of surgical site infection for clean-contaminated or dirty procedures.
“The literature in equine practice further supports the concept that prolonged antimicrobial usage (single prophylactic dose or 72 vs. 120 hours) did not yield additional benefits; furthermore, prolonged administration is known to contribute to development of complications such as colitis and Salmonella shedding,” Rockow et al. wrote in their 2023 study.
To generate additional data, Rockow et al. retrospectively evaluated medical records of 608 celiotomies to determine if pre-, intra-, or postoperative antibiotics were associated with risk of incisional infections. In that analysis, duration of postoperative antibiotics varied widely from no antibiotics in 0.8% of the cases to a mean of 3.9 days. The rate of incisional infections was low, however, at only 6.4%, prompting the authors to note, “detecting statistical differences would be difficult due to the low infection rate overall.”
The retrospective study by Crabtree et al. (2025) also found no improvement in the rate of incisional infection with prolonged antibiotics. In that study, 187 horses undergoing celiotomy were divided into three groups based on duration of antimicrobial therapy: ≤ 24 hours, 1-3 days, and > 3 days. The overall infection rate was 12.8%, with no difference between the groups, although the study was small and may have lacked power.
Taking a prospective approach, the research group of Kate Christie, DVM, MSc, DACVS (LAIM), a stakeholder veterinarian at Rood & Riddle Equine Hospital in Lexington, Kentucky, enrolled horses undergoing clean-contaminated emergency celiotomies treated with either pre- and intraoperative antibiotics only or those also treated with postoperative antibiotics (for 72 hours). Surgical site closure and postoperative incision protection was standardized.
Christie reported that the prevalence of incisional infections in the horses with only pre- and intraoperative antibiotics was 16% (6/37 horses) and 0% in the 35 horses that also received postoperative antibiotics. This difference was significant, contradicting the research team’s hypothesis that there would be no difference in incision infection prevalence.
This finding suggests a potential benefit to continuing antimicrobials beyond the pre- and intraoperative dosing in horses undergoing exploratory celiotomy, which also strays from their hypothesis and conclusions made by the other research groups.
According to the study, participating surgeons were hesitant to enroll cases that might not receive the postoperative antibiotics. “It was clear that a number of surgeons at the study location had limited comfort with discontinuing antimicrobials prior to 72 hours for most clean-contaminated procedures,” wrote Christie.
This postoperative antibiotic use contradicts research in human medicine where patients receive no antibiotics after the incision is closed and in small animal medicine where antibiotics are discontinued within 24 hours of surgery.
Additional studies are required, but achieving appropriate sample sizes has proven to be challenging.
Manuka Honey
In 2024, Gandini et al. published a study showing that applying a pectin-honey hydrogel to the linea alba during routine closure of the abdomen following laparotomy reduced the prevalence of incisional infections. Manuka honey has antimicrobial activity and beneficial effects on wound healing, including improved angiogenesis and reduced healing times. The research team selected a pectin-honey hydrogel rather than liquid honey because it reportedly remains at the site longer and is easier to apply during surgery.
The study included 36 horses presenting for colic surgery. Randomly, 18 horses had a pectin-honey hydrogel applied to the sutured linea alba before routinely closing the remainder of the abdomen. An abdominal stent was placed over the skin for five days in all horses. Complete blood counts were performed on all horses for the first three days postoperatively, and antimicrobials were administered until values returned to normal.
The team monitored incisions closely and diagnosed infection based on the presence of serosanguinous drainage for more than 24 hours after surgery or the presence of purulent discharge. The overall rate of incisional infections was 19.4%, but infection occurred in only one horse (5.5%) in the group treated with the pectin-honey hydrogel and six of the 18 horses (33.3%) in the control group. Thus, horses in the control group had an 8.5-fold increased risk of incisional infection.
The pectin-honey hydrogel appeared safe, with no macroscopic evidence of adverse effects such as inflammation or foreign body reaction.
Bandaging
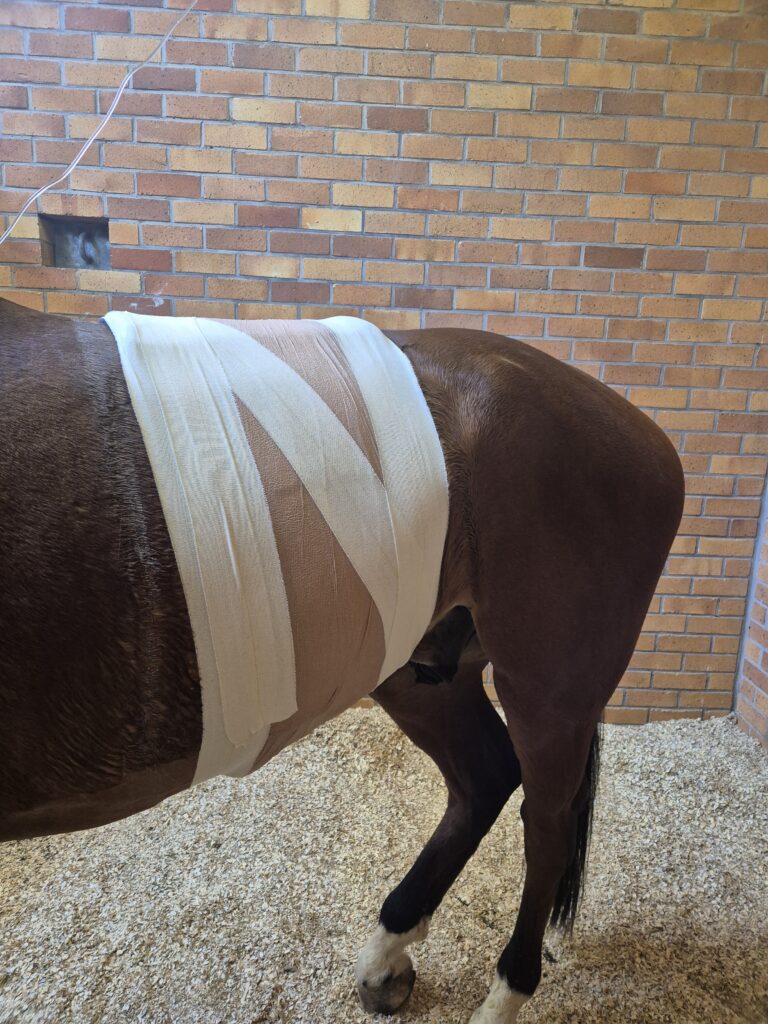
Isgren et al. evaluated the effect of a sutured-on stent dressing to help protect the incision during recovery and reduce the prevalence of infection. Minimizing bacterial contamination of the incision during the early postoperative period, particularly during anesthetic recovery, might decrease the risk of incisional infections. As such, the research team evaluated the effect of a commercially sutured-on stent dressing compared with a standard adhesive dressing (both three-layer abdominal bandages) placed for recovery on incisional infections (defined as purulent discharge from the incision or more than 24 hours of serous discharge accompanied by pain, localized swelling, heat, or erythema) after emergency laparotomy.
Following recovery, the bandages were immediately replaced with new abdominal dressings and bandages that were changed every 48 hours (or sooner if evidence of exudate through the bandage). Perioperative antimicrobials were administered according to the standard hospital practice and modified based on surgeon’s preference.
This randomized controlled trial included 352 horses: 167 in the stent group and 185 in the control group. The overall prevalence of incisional infections was 28.7%, occurring at a mean of 9.7 days postoperatively (standard deviation was 4.6 days) with no difference in infection rate between the two groups. Of interest, the prevalence of incisional infections occurring during hospitalization was 18.8%, showing that even after discharge, incisions must be carefully monitored because infections can still develop (up to 30 days postoperatively).
“These numbers are unfortunately still very high, and that is why I believe that incisional infection remains an important topic for future research,” says Griessel. “There is disagreement between authors in the literature regarding how and for how long the incision should or should not be covered postoperatively.”
Griessel places a stent bandage over the incision for recovery, followed by a belly bandage for 14 days postoperatively.
“We find that this protects the incision if the horse were to lie down or display any colic signs during this critical time when the incision is healing,” he explains. “It is our impression that the belly bandages also help reduce the postoperative edema that may develop around the incision postoperatively.”
Future prospective research investigating incisional protection might benefit from comparing more standardized application of stents and abdominal bandages, says Griessel.
Negative Pressure Bandages
Salciccia et al. (2024) described closing the linea alba with vertical U mattress tension sutures using polyglactin 910 apposed by either interrupted or simple continuous sutures. In their hands, this technique resulted in a surgical site infection prevalence of only 5.3%, the lowest reported in the literature reviewed for this article. Those surgeons also used negative pressure bandages in cases considered highly susceptible to incisional infections (e.g., repeat celiotomies or incisions greater than 30 cm in length).
While the negative pressure bandages were easy to apply and had no detrimental effects, “the potential prophylactic benefit of this therapy needs to be confirmed in a larger group” and should include a control group. “There have been some interesting studies in people with wound vacs,” adds Hendrickson. “The horse is a bit more challenging to keep negative pressure, but it seems like it would be worth working on more.”
Summary
Incisional infections increase treatment costs, might require additional or extended hospitalization, and can progress to abdominal herniation, which might limit future athleticism.
“Time is trauma,” says Hendrickson. “The longer the incision is open and the more trauma to the incision edges, the more likely an infection takes hold. Medical-grade honey, local raw honey, or polyhexanide gels can be used after surgery, and belly bandages for recovery that are removed when the horse stands are beneficial. Local therapy using antimicrobial impregnated dressings over the incision also seems to reduce the chance of surgical site infections.”
Related Reading
- Antimicrobial Stewardship With Honey
- Colic Surgery’s Impact on Show-Jumping Horses’ Careers
- Evidence-Based Antiseptics & Dressings for Equine Wounds
Stay in the know! Sign up for EquiManagement’s FREE weekly newsletters to get the latest equine research, disease alerts, and vet practice updates delivered straight to your inbox.

![[Aggregator] Downloaded image for imported item #19769](https://s3.amazonaws.com/wp-s3-equimanagement.com/wp-content/uploads/2026/05/31141823/EDCC-Unbranded-11-scaled-1-768x512.jpeg)

