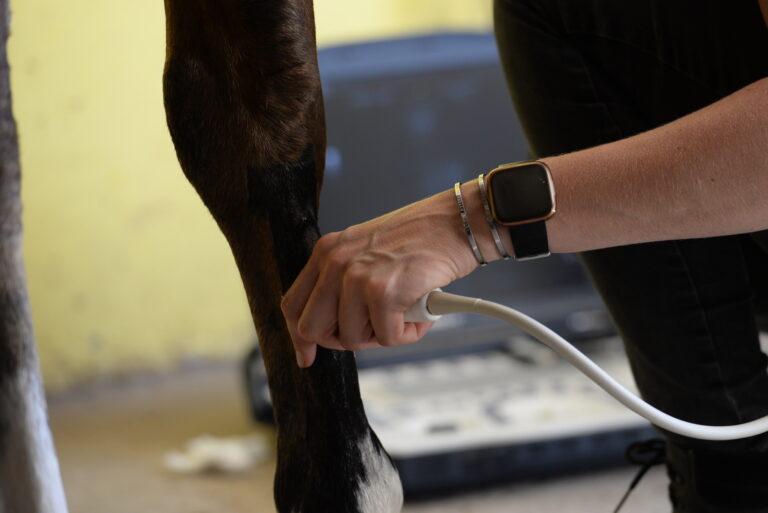
Ultrasound imaging is based on the properties of sound waves and how they travel through the variation of tissue densities. Every tissue has unique acoustic properties that allow us to define the different structures. The structure of tendons and ligaments has important implications in ultrasound imaging.
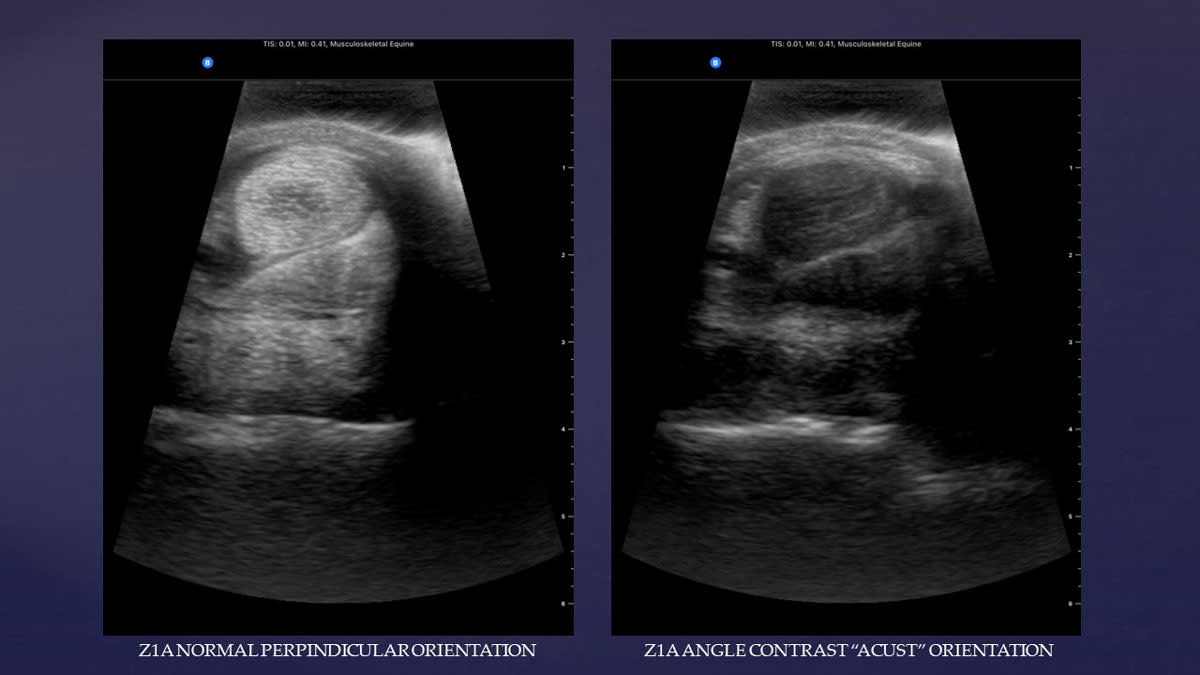
When performing longitudinal imaging, the fascicular architecture of these structures is seen as multiple tightly packed echogenic parallel lines. However, in the transectional plane, the fascicles are elucidated as echogenic dots and lines. When the ultrasound beam is perpendicular to the orientation of the fascicles, the maximum return echo occurs and they will show as brightly hyperechoic.
Anisotropy is a sonographic artifact described as “the angle-dependent appearance of tissues.” If the angle of the transducer is altered proximally or distally from perpendicular, the ultrasound image appearance of tendons and ligaments will change from hyperechoic (lighter) to hypoechoic (darker). If the sonographer is not experienced in this property of ultrasound, this might lead to a false diagnosis of a tendinopathy or desmopathy.
However, anisotropy and its properties can also be harnessed as a very useful ultrasound tool.
Dr. Jean-Marie Denoix of the International Society of Equine Locomotor Pathology (ISELP), has coined the term “angle contrast ultrasound technique” or “ACUST” imaging. The terms on-beam and off-beam have also been used.
Again, tendon and ligament fibers become significantly hypoechoic (darker) depending on the angle used.
Tissues with a different fiber organization—such as fibrocartilage, fat, muscle and scar tissue—will remain echogenic regardless of beam angle, allowing imaging enhancement of these different tissues.
Areas of fiber disruption and fluid are hypoechoic or anechoic in both normal orientation and angle contrast orientation.
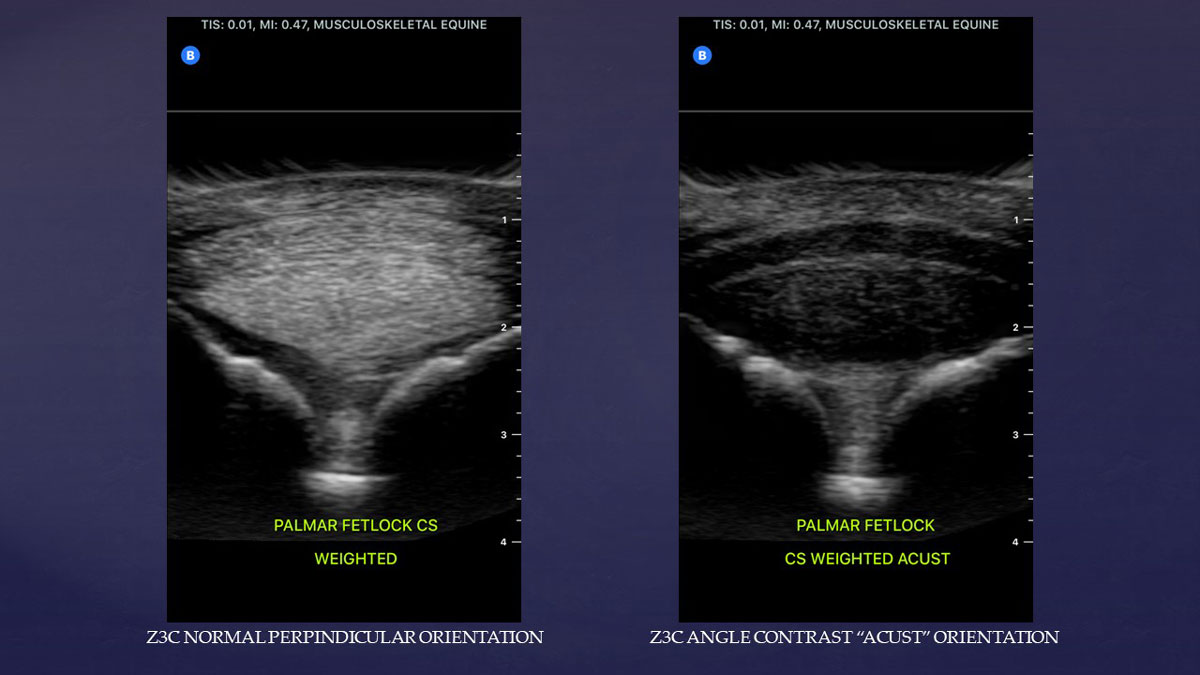
This allows us to fine tune our evaluation of structures such as the fibrocartilage layers of the superficial digital flexor tendon in the distal metacarpal and metatarsal regions (see image below), the mannica flexorum, or the suspensory ligament.
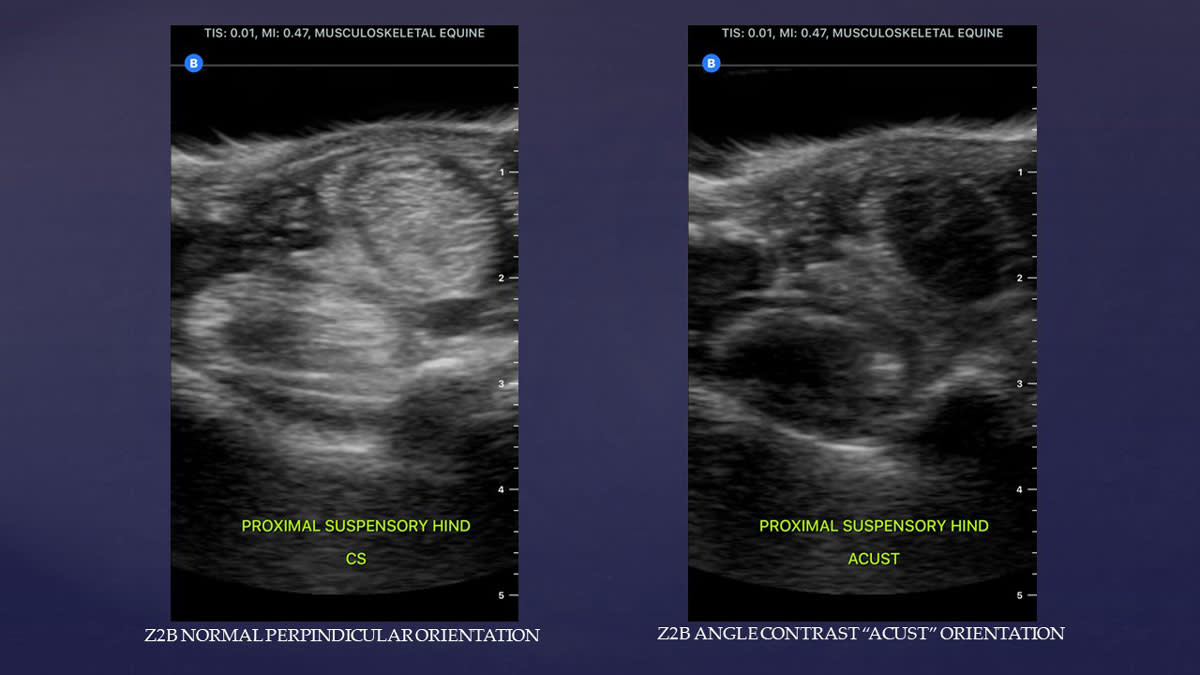
The suspensory ligament body is a vestigial muscle from evolution, and as such, contains defined areas of fat and muscle nicely visible in ACUST imaging. They appear as comma-shaped islands within the cross section of the suspensory body (see image below). If the ligament fibers are injured and enlarged, they compress these areas of fat and muscle, significantly altering their appearance.
As stated previously, scar tissue will remain echogenic in ACUST imaging, allowing it to be visualized within structures that should be hypoechoic in the ACUST orientation. As a result, angle contrasting allows practitioners to delineate acute versus chronic lesions.
In situations where periligamentous and peritendinous fibrosis occurs, ACUST imaging allows us to more accurately define tendon and ligament borders. ACUST imaging even allows us to define the outer paratenon layer of a tendon structure, as it is comprised of a thin layer of loose fatty connective tissue.
The author finds it useful to display a split screen when performing a sonogram sequentially through the length of a tendon or ligament structure. Initially displaying a normal perpendicular image on the left side of the screen and an ACUST image in the exact same location on the right side of the screen allows comparison. The image is acquired, then the right-hand image is replaced with a longitudinal image in the same location and acquired again.
In conclusion, the anisotropic properties of ultrasound must be understood, and care must be taken to avoid misdiagnoses because of these properties. At the same time, these properties should be used routinely as a tool to more accurately define both normal and abnormal or pathologic anatomy.
About the Author
Cooper Williams, VMD, DACVSMR, Certified ISELP Instructor, grew up in Cecil County Maryland, where he learned to play polo and train polo ponies with his family. He ultimately obtained a five goal rating and played professionally for five years. In the summer of 1981, he was a member of the United States polo team that competed throughout England. He coached the Valley Forge Military Academy polo team from 1981 to 1985. In 1984, he graduated with honors from the University of Pennsylvania School of Veterinary Medicine. He accepted a post graduate internship at Delaware Equine Center, where he developed their ultrasound imaging program. In 1987, he moved to Maryland where he worked for two years at Maryland Equine Center, also developing their ultrasound program. In 1989, Williams started his own practice, focusing on diagnostics and sports medicine in equine athletes. After three years of rigorous study, learning in depth about advanced diagnostic imaging, Williams passed his examination and was certified by the International Society of Equine Locomotor Pathology (ISELP) in 2009 and has continued on as a certified instructor with ISELP, teaching other equine veterinarians all over the world. Cooper is one of a small group of veterinarians in the world who is certified by the International Society of Equine Locomotor Pathology in advanced ultrasound imaging. In August 2014, Williams successfully passed his examination and is officially a Diplomate of the American College of Veterinary Sports Medicine and Rehabilitation. There are only a small group of veterinarians in the world that now can claim they are a specialist in sports medicine and rehabilitation. He is an active member of the North American Regenerative Medicine Association as well as being on the veterinary advisory board for ACell, Inc., a tissue engineering company.
Williams is a paid advisor for Butterfly Network.