This article originally appeared in the Winter 2024 issue of EquiManagement. Sign up here for a FREE subscription to EquiManagement’s quarterly digital or print magazine and any special issues.
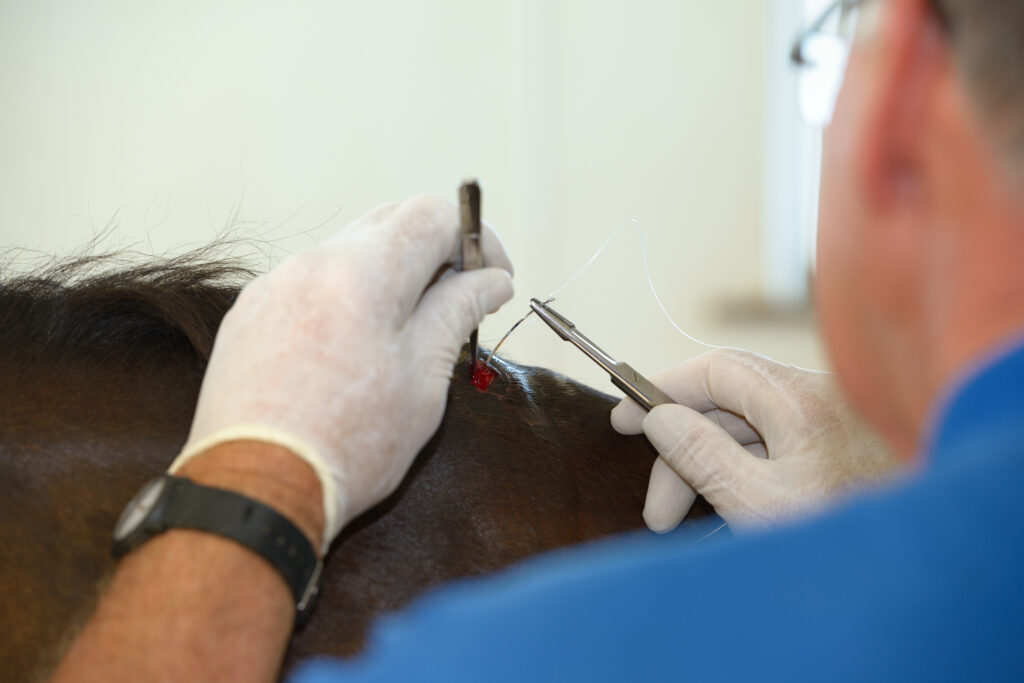
Wound healing in horses can be challenging for reasons ranging from infection risk to lack of soft tissue. Research into alternative methods in human medicine might lead to the development of wound healing options and products for animals, as well. A couple of resources might eventually provide opportunities to improve equine wound outcomes. Here are potential options to watch for.
Melanin
Melanin has important protective properties for skin, such as absorbing ultraviolet light and acting as a free radical scavenger for wounds subjected to oxidative stress. A dermatologist and an MD from Northwestern University collaborated on the use of melanin to accelerate skin tissue repair by removing reactive oxygen species. Melanin cannot be extracted in a pure form from natural sources because of contaminants, so they bioengineered a topical form of synthetic melanin particles (SMP) in the lab.1
Their studies in mice demonstrated accelerated healing following skin damage from ultraviolet or chemical exposure. While the SMPs didn’t penetrate the stratum corneum, they did have beneficial effects: Both edema and eschar attachment time shortened, with faster reductions of both wound size and depth. Tests on injured human tissue discarded following plastic surgery demonstrated favorable responses to SMP treatment. The researchers reported that “SMPs were found to modulate the immune response by increasing the number of reparative and anti-inflammatory cells in the wound area and regulating the systemic immune response.”
Melanin not only binds to reactive oxygen species (ROS), but it also improves the efficacy of skin’s native antioxidant system. It increases superoxide dismutase (SOD) activity, an inherent defense mechanism against ROS—this further helps recover skin SOD levels. SOD activity facilitates the expression of matrix metalloproteinases (MMP9) that at low levels result in shallower injuries with more rapid healing. The researchers said a big surprise was how using SMPs “orchestrates the immune system to repair skin.”
SMP efficacy does not appear to depend on cellular uptake by macrophages or other cells. Within two to three days of skin injury, erythema and tissue swelling both decreased. Angiogenesis increased, and apoptosis decreased. Dermal and epidermal tissues recovered by Day 16.
The researchers report that SMPs are biocompatible and nonallergenic. FDA studies are not yet available to ascertain safety and regulatory criteria. The objective is to provide alternative wound treatment for skin burns caused by radiation, chemical, or ultraviolet exposure. SMPs might also help mitigate adverse skin effects from chemotherapy.
Tissue Adhesive
Use of an ethyl 2-cyanoacrylate tissue adhesive in humans is associated with less discomfort and shortened healing time. It also provides a physical barrier to environmental contaminants, reduces dehiscence, and offers greater resistance to exudates. The authors of a Brazilian study recently compared the healing efficacy of tissue adhesive (AG) to nylon sutures (SG) on horses’ neck and croup wounds.2
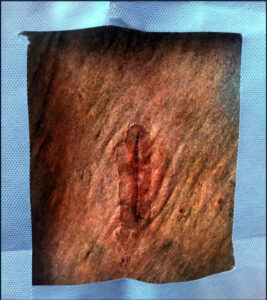
In the study, eight horses received incisions about 3 inches long on both sides of the neck. The researchers used SG for repair of the left side and AG (Epiglu) for the right side. They performed the same procedure at a different time on both sides of the croup, again with SG on the left and AG on the right. They evaluated the wounds on Days 1, 3, 7, 10, and 12 using photographs and objective and subjective means—sensitivity to touch, tissue consistency, volume increase, temperature changes, secretion or granulation tissue at the site, healing process, and signs of rejection of the biomaterial. On Day 12, the authors obtained a piece of “healed” skin for microscopic examination.
Microscopic exam of skin samples from Day 12 revealed more inflammatory cells, fibrosis, and collagen deposition within the sutured (SG) wounds than with tissue adhesive. The researchers suggested this is because of greater tissue manipulation when applying sutures and nylon acting as a foreign body. AG wounds showed more tissue reaction of sebaceous and sweat glands around the scar, possibly due to contact dermatitis from the glue.
Both sutured and adhesive-repaired wounds had similar findings regarding touch sensitivity, temperature increase, and presence of secretions, crusts, and granulation tissue. For both neck and croup lesions, it took longer for the sutured wounds to heal than those closed with tissue adhesive.
While the AG material was easy to apply and caused no discomfort, the researchers note that in cases of heavy bleeding it is difficult to use because AG “polymerized rapidly on contact with blood.” While this is beneficial for hemostasis, it limits satisfactory wound synthesis, thereby leading to a greater potential for dehiscence. Wounds closed with sutures had no dehiscence in either neck or croup location whereas AG had 50% dehiscence, mostly occurring between Days 1 and 3. Of the wounds that dehisced, 37.5% were total and 12.5% were partial.
The authors reported that in this kind of large wound, using tissue adhesive alone without relaxing sutures has the potential to result in dehiscence. They recommend using subdermal sutures to greatly improve tissue apposition and healing when using tissue adhesive in relatively large wounds.
The manufacturer claims on tissue adhesive assert that the adhesive self-releases within five to 10 days. In this study, adhesive parts remained by Day 12 with nearly all the adhesive still present in some horses by the end of the study.
The authors concluded that the tissue adhesive provides good biocompatibility but did not give good results in areas of skin tension; efficacy can be improved by using relaxing sutures. In other respects, the tissue adhesive yields benefits because it serves as a physical barrier to contamination, doesn’t need to be removed postoperatively, and creates less of an inflammatory response than nylon sutures.
References
- Biyashev D, Siwicka ZE, Onay UV, et al. Topical application of synthetic melanin promotes tissue repair. NPJ Regen Med Nov 2023, vol. 8; 61; DOI: 10.1038/s41536-023-00331-1
- de Oliveira GL, Ambrizi DR, Reginato GM, et al. Use of Ethyl 2-cyanoacrylate in Skin Synthesis in Horses — Evaluation of Efficacy and Biocompatibility. Acta Scientiae Veterinariae 2024, Vol 52; DOI: 10.22456/1679-9216.129991
Related Reading
- Chlorhexidine Flush: Potential Treatment for Septic Arthritis in Horses?
- Responsible Antimicrobial Usage in Horses
- Equine Pathogens’ Susceptibility to Different Wound Dressings
Stay in the know! Sign up for EquiManagement’s FREE weekly newsletters to get the latest equine research, disease alerts, and vet practice updates delivered straight to your inbox.

![[Aggregator] Downloaded image for imported item #18375](https://s3.amazonaws.com/wp-s3-equimanagement.com/wp-content/uploads/2025/09/30140031/EDCC-Unbranded-26-scaled-1-768x512.jpeg)


